Understanding the Warning Signs: How to Recognize Symptoms of a Mild Stroke
Strokes stand as one of the leading causes of long-term disability and mortality globally. The term ‘stroke’ encompasses a range of conditions characterized by an interruption of blood flow to the brain, leading to the death of brain cells. However, a precursor to more severe types is a mild stroke or transient ischemic attack (TIA). These events are warning shots, sudden but brief blockages in the brain’s blood vessels that resolve without causing permanent damage.
What is a Mild Stroke?
A mild stroke, or transient ischemic attack (TIA), may be considered a ‘mini-stroke,’ but there is nothing minor about its significance. A TIA presents with stroke-like symptoms that typically last for less than 24 hours before disappearing. While not causing permanent brain damage, a TIA is often a sign of potentially significant strokes in the future. The temporary nature of a TIA’s symptoms can paradoxically pose a danger; individuals might not take them as seriously as they should. Differing from other types of stroke due to its short duration, a TIA nevertheless requires the same level of emergency medical response to reduce the risk of a subsequent, more severe episode. Understanding the warning signs associated with mild stroke symptoms is essential, as prompt recognition and response could mean the difference between a full recovery and lasting consequences.
Identifying the Symptoms of a Mild Stroke
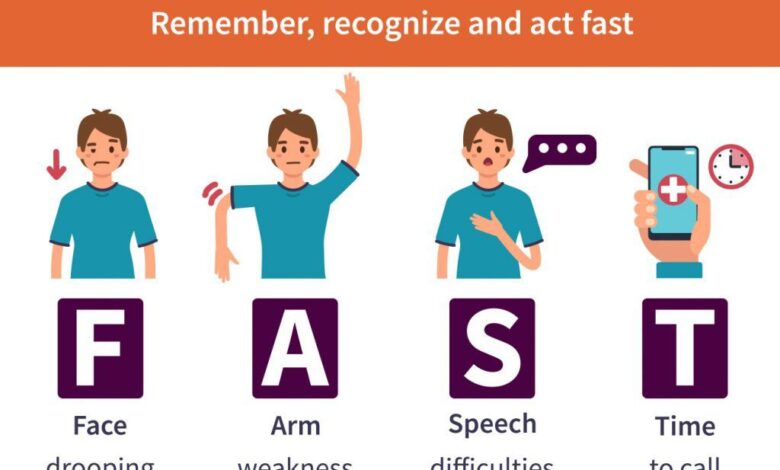
Recognizing the symptoms of a TIA can be challenging because they can be surprisingly brief. One moment, an individual might experience weakness, numbness, or paralysis in the face, arm, or leg—usually on one side of the body. There might be sudden confusion, trouble speaking or understanding others, dizziness, loss of balance, or an unexplained severe headache. Vision problems, such as blurred or double vision, can also occur. These stroke awareness initiatives highlight the urgency of recognizing these fleeting symptoms—they could present a narrow window for preventing more serious health issues.
Risk Factors for a Mild Stroke
Several risk factors increase the likelihood of experiencing a TIA. High blood pressure is the leading cause of stroke; it damages blood vessels, leading to blockages. Other common risk factors include heart disease, diabetes, and high cholesterol. Lifestyle choices—such as smoking, excessive alcohol consumption, a diet high in saturated fat, and physical inactivity—also play a crucial role. Recognizing and managing these factors can help reduce the chances of a TIA or a major stroke. Importantly, anyone can be at risk; however, African Americans and older people have a higher propensity for TIAs due to specific health and genetic variables.
The Role of Diet and Exercise in Stroke Prevention
Diet and exercise are two controllable factors significantly impacting the prevention of mild strokes. A balanced diet rich in fruits, vegetables, whole grains, and reduced saturated fats, salt, and cholesterol can help lower blood pressure and cholesterol levels, decreasing stroke risk. Physical exercise, even moderate, aids in maintaining a healthy weight, reducing blood pressure, and improving overall cardiovascular health. Integrating regular daily activities, such as brisk walking, cycling, or swimming, can be preventive solid medicine against strokes.
Long-Term Effects of Mild Strokes
Although symptoms of a TIA are temporary, they can indicate significant underlying health issues that, if left unaddressed, can lead to severe strokes with long-lasting effects. These can include permanent muscle weakness, difficulty speaking, memory loss, and emotional difficulties. Early diagnosis and treatment are crucial for minimizing the potential long-term effects of a TIA. Post-TIA care often includes rehabilitation services designed to improve any deficits in strength, coordination, speech, and cognitive ability.
Innovations in Stroke Detection and Treatment
The landscape of stroke detection and treatment has seen impressive innovations in recent years. Technological advancements have led to more precise imaging methods, enabling quicker and more accurate stroke detection. In the realm of treatment, pharmaceutical developments offer new medications that can better prevent blood clots without undue risk of bleeding. Research continues to drive improvements in treatment protocols and rehabilitation practices, enhancing the long-term outcomes for stroke survivors.
Personal Stories: Living with the Effects of a Mild Stroke
Survivors of TIAs often share compelling stories of how recognizing and responding to symptoms made lasting differences in their health outcomes. These stories offer a unique insight into the real-life impact of TIAs and highlight the importance of public awareness. Personal narratives also showcase the recovery journey, emphasizing the resilience of individuals and the crucial support of healthcare providers and loved ones throughout the process.
Understanding the Medical Response to a TIA
Should a TIA occur, the first action should be to call emergency services—time saved is brain saved. Medical professionals will promptly work to assess the situation, using diagnostic tools such as CT or MRI scans to determine the cause and extent of the stroke. Depending on the results, treatment may involve medications like blood thinners, statins, or anticoagulants to prevent clots. In some situations, surgical options, such as carotid endarterectomy or stenting, are necessary. The advancements in stroke prevention and recovery mean that there is a broader range of options for treating and rehabilitating patients who have experienced TIAs.
Preventive Measures and Regular Health Checks
Proactive prevention is fundamental in reducing the risk of strokes. This includes adopting a healthy lifestyle and managing risk factors like blood pressure and cholesterol levels. Regular health screenings can detect the early signs of conditions that increase the risk of a stroke. Additionally, discussing family medical history with a healthcare provider can help identify genetic predispositions and form an individualized prevention plan. Individuals with a healthcare team can establish effective strategies supporting a brain-healthy life.



